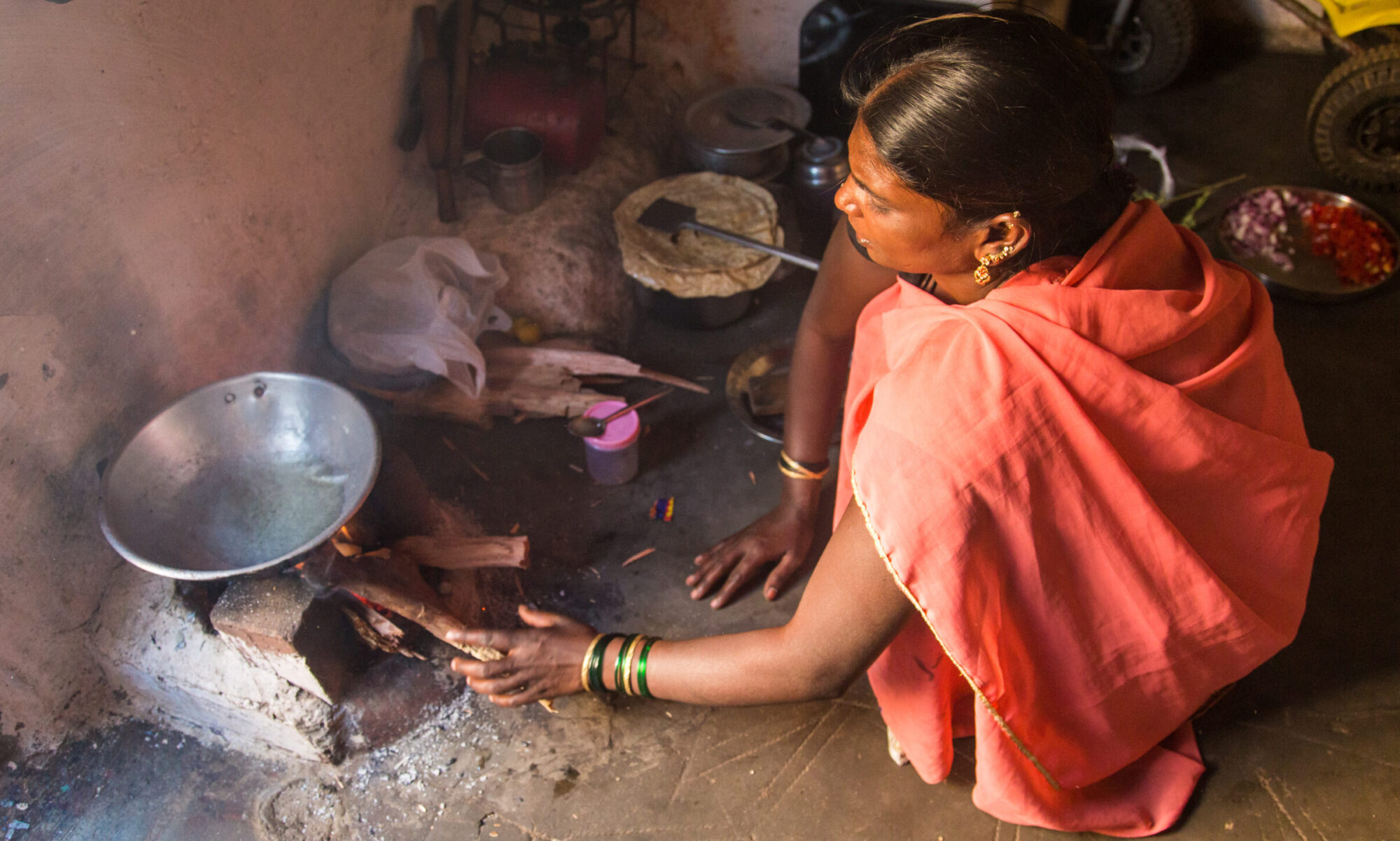On April 3, 2023, Megha Thakur succesfully defended her thesis entitled ‘low-smoke chulha and health consequences in Indian slums’.
The dissertation can be accessed here: https://cris.maastrichtuniversity.nl/en/publications/low-smoke-chulha-and-health-consequences-in-indian-slums
Household air pollution (HAP) is one of the leading environmental and public health concerns globally. Resulting from the inefficient combustion of solid fuels (i.e. wood, coal, charcoal, crop waste, dung), and kerosene, HAP disproportionately affects the poorest and marginalized populations, including women and children. Nearly 2.4 billion people (around a third of the global population) still depend on polluting fuels and technologies for cooking. Women and children bear the brunt of HAP because of the amount of time they spend indoors. Both long- and short-term exposure to HAP has impacts on health. Chronic exposure over the lifetime increases the risk for non-communicable diseases such as respiratory cancers, cardiovascular disease, stroke, and chronic obstructive pulmonary disease (COPD). Short exposure can already lead to acute health outcomes such as pneumonia and adverse
pregnancy outcomes such as stillbirth, preterm delivery, and low birth weight.
The main burden of HAP can be seen in low-resource settings. Use of solid fuels in India is not only common in the rural homes but also in the slum areas as well as in a majority of smaller cities and towns. However, most of the studies on HAP are conducted in rural areas with little evidence from urban areas. In 2018, 86.6 million people in urban India were still primarily dependent on polluting fuels and technologies for cooking. Slum residents face a disproportionate risk to HAP because of the dense population often residing in poorly ventilated houses. Although a direct switch to clean fuels remains the ideal solution, it is still a challenge. Having identified these challenges, WHO guidelines recommend more advanced combustion cookstoves (stoves that maximize combustion efficiency) offering some health benefits which should be prioritised in the transition to clean cooking solutions. Project Exhale aimed to reduce the levels of HAP and improve the respiratory health of women and children in urban slums by installing a locally manufactured improved cookstove (ICS).
The aims of Megha’s research were:
1) To conduct a systematic review and meta-analysis of the impact of ICS on women’s and child health in low- and middle-income countries;
2) To conduct a cross-sectional study among and health; and
3) To evaluate the effectiveness of an ICS on the health of women and children in slums in a trial.